Strong bone holds your dental implant in place. Weak bone puts it at risk. When you plan for implants, bone density is not a small detail. It shapes every step of your treatment. It affects what type of implant you need, how many visits you will have, and how long healing will take. It also affects how long your implant will last. If you have missing teeth, long-term dentures, gum disease, or osteoporosis, your bone may already be thin. You may still qualify for implants. You just need careful testing and a clear plan. An implant dentist Queens will measure your bone, study your medical history, and choose safe options. This blog explains why bone density matters, what your scan results mean, and what choices you have if your bone is weak. You deserve a stable bite and a confident smile.
What bone density means for your jaw
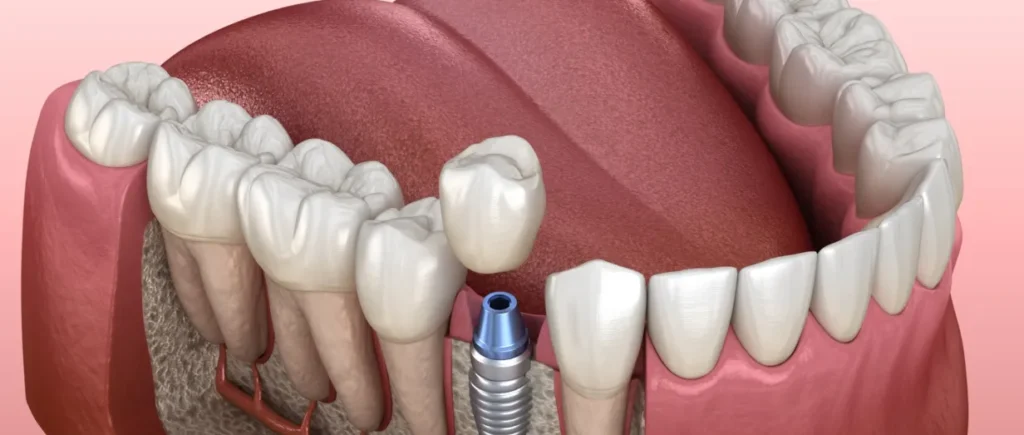
Bone density is the amount of mineral content in a section of bone. High-density bone feels firm. Thin bone feels soft. Your jawbone holds each implant post like soil holds a fence post. If the soil is firm, the post stands straight. If the soil is soft, the post leans or fails.
Three key points guide planning.
- Dense bone grips the implant and helps it heal.
- Thin bone raises the chance of movement and failure.
- Proper testing lets your dentist adjust the plan early.
The National Institute of Arthritis and Musculoskeletal and Skin Diseases explains how low bone mass develops over time and how common it is.
Who faces a higher risk of low jawbone density
Anyone can lose jawbone. Some people face a higher risk. Your dentist looks at three main groups.
- People with missing teeth for many years
- Denture users who feel loose or rubbing plates
- People with known bone loss or osteoporosis
Tooth loss starts a slow chain reaction. The bone under the missing tooth no longer feels the chewing forces. Over time, the body removes some of that unused bone. Long-term, the ridge of bone shrinks. Dentures can speed this loss if they move or grind the gums.
Whole body bone loss also matters. The jaw is part of your skeleton. If your spine or hip shows low bone mass, your jaw may be thinner than average. The U.S. Centers for Disease Control and Prevention shares data on bone health in adults. You can see national numbers at the CDC Second Nutrition Report on Bone Minerals.
How your dentist checks your bone
Your dentist does not guess about bone density. You get tests. Each test answers a different question.
- Dental X-rays show the height of the bone and the basic shape.
- 3D cone beam CT scans show width, density, and nerve paths.
- Medical bone scans or DEXA reports show overall bone health.
First, your dentist reviews your health history. Medications for osteoporosis, cancer, or immune conditions change healing. Next, you get images. A 3D scan lets the dentist measure exact millimeters of bone at each implant site. You may hear letters like D1 or D2. These labels describe how dense the bone is. Dense front jawbone supports implants quickly. The soft upper back jawbone needs more care.
Bone density and implant choices
Bone density shapes almost every choice in your treatment plan.
- Implant size and shape
- Number of implants
- Healing time before new teeth attach
Here is a simple comparison of how bone types guide planning.
| Bone type | Common jaw location | Planning effect | Typical healing time before full load |
|---|---|---|---|
| High density bone | Front lower jaw | Shorter implants can still hold well. Fewer implants may be needed. | 3 to 4 months |
| Medium density bone | Front upper jaw | Standard implant size. Normal number of implants. | 4 to 6 months |
| Low density bone | Back upper jaw | Longer or wider implants. Possible bone graft or sinus lift. | 6 to 9 months |
| Very thin bone | Areas with long term tooth loss | Staged bone grafting. Use of fewer, longer implants or special designs. | 9 months or more |
When bone is thin, you still have choices
Weak bone does not always mean no implants. It means more steps. You and your dentist can talk through three common paths.
- Bone grafting with delayed implants
- Sinus lift for the upper back jaw
- Use of longer or angled implants in stronger parts of the jaw
First, bone grafting adds bone or bone like material to thin spots. Your body then grows new bone around it. This can restore height and width where teeth have been missing. Second, a sinus lift gently raises the sinus floor and adds bone so implants do not enter the sinus space. This is common for upper molars. Third, some full arch plans place implants at angles into stronger front or side bone. This can avoid some grafts.
Each option adds time. It also lowers the risk that the implant will fail or feel loose. Careful staging is safer than rushing.
How bone density affects healing and long-term success
After surgery, your bone grows onto the implant surface. This bond holds the implant firm. Dense bone forms this bond with fewer surprises. Thin bone needs more healing time and lighter bite forces.
Your dentist may protect healing in three ways.
- Use temporary teeth that put less pressure on the implants.
- Ask you to avoid chewing hard food on the implant side at first.
- Schedule closer follow-up visits to track progress.
Long term, strong bone supports a calm, even bite. Weak bones may shrink more if you grind your teeth or smoke. You protect your bone when you clean your mouth each day, keep checkups, and manage habits like clenching.
How to prepare for your implant visit
You can help your dentist plan by sharing clear information.
- Bring a list of all medications and supplements.
- Share past fractures or bone test reports.
- Tell your dentist about smoking or vaping.
Also ask direct questions.
- How strong is my jawbone in each implant site
- Will I need bone grafting or a sinus lift
- How long will healing take before I use my new teeth fully
Bone density shapes your implant path, but it does not define your future. With clear tests, honest talks, and a careful plan, you can move toward stable teeth that let you eat, speak, and smile with steady comfort.